This week in healthcare news, we look at a new, futuristic skin implant that changes color to mimic a skin mole if it detects rising calcium levels, a potential sign of cancer. Addressing the opioid crisis is again in the news, as is the rising cost of prescription drugs. And lastly, Cigna faces litigation that it enacted a cost-shifting scheme to divert administrative charges. This and more in the Innovation Partners BioBlog.
How to ensure bundled payments coexist with ACOs
Overlap between two payment models, bundled payments and accountable care organizations (ACOs), need to be resolved, according to researchers. Medicare favors both alternative payment models but there is overlap between the two. Bundled payments deal directly with hospitalizations and post-acute care, whereas the MSSP rewards care quality and costs over an annual time frame.
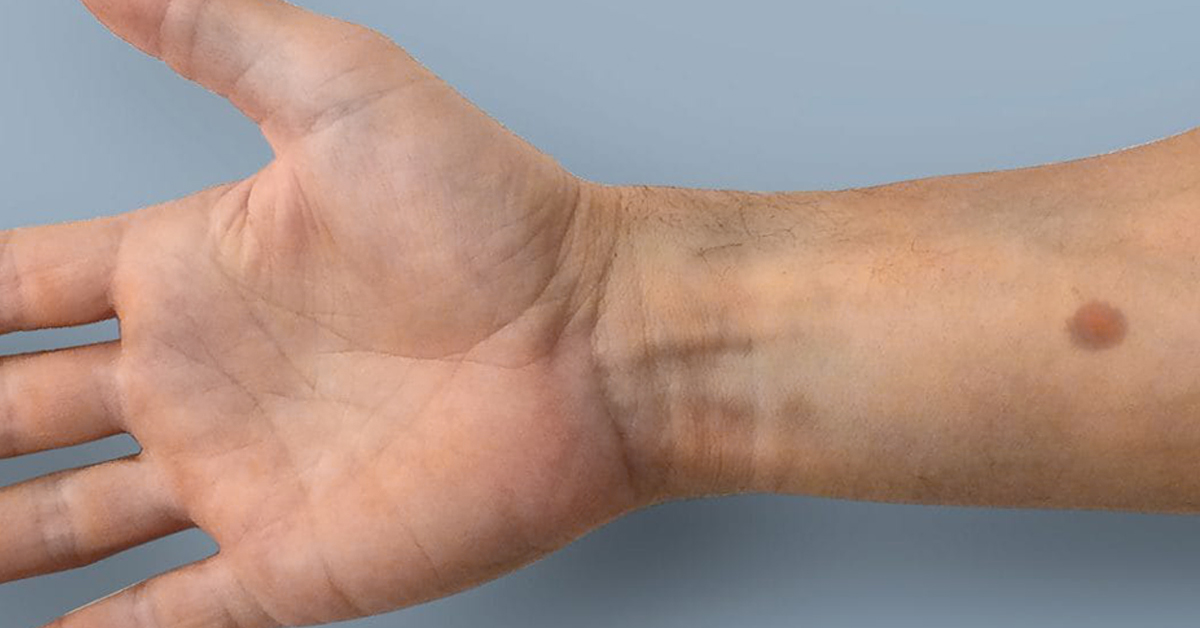
Implant will show when cancer is present by generating artificial mole on skin
A new implant could help detect skin cancer. The implant works by detecting rising levels of calcium in the body. Rising calcium levels trigger the production of melanin, the body’s tanning pigment, turning the implant into an artificial mole. Swiss scientists from the university ETH Zurich say the device can recognise the four most common types of cancer – prostate, lung, colon and breast cancer – at a very early stage of tumour development. The desire is to make early detection easy with the hope of enacting treatment plans swiftly once cancer is detected.
Trump to give speech on lowering drug prices this month
The White House stated that President Trump will deliver a speech on April 26th addressing the need to lower drug prices. Trump has called for making drugs more affordable. No new policies will be unveiled during the speech.
DEA to share prescription drug data with 50 attorneys general, crack down on drugmakers
The DEA reached an agreement with 50 attorneys general this week to share information in an effort to support ongoing investigations into prescription drugs. Details of the data sharing agreement are murky, but the DEA will share data from its Automation of Reports and Consolidated Orders System (ARCOS), which collects 80 million prescription drug transactions from manufacturers and distributors each year.
Backed by medical groups, value-based payments for opioid addiction treatment could be imminent
The American Society of Addiction Medicine (ASAM) and the American Medical Association (AMA) announced today a collaborative value-based payment model for opioid addiction treatment. The announcement came today amidst discussions with Congress on how to manage the opioid addiction crisis. The organizations have said that medication-assisted treatment is underused. Limited insurance coverage, a shortage of qualified physicians and a lack of access to addiction specialists for many patients contribute to its under utilization.
Cancer hospitals push for Medicare CAR-T payments
Lobbyists for several cancer hospitals are urging Medicare officials to create a new set of payments for CAR-T treatments. The new treatments are expensive and use the body’s own immune cells to attack cancer. Two CAR-T treatments, Kymriah, made by Novartis and Yescarta, made by Gilead Sciences, are FDA approved.
Class-action lawsuit accuses Cigna of cost-shifting scheme to divert administrative charges
Cigna faces a lawsuit alleging a cost-shifting scheme to divert administrative charges. The class-action lawsuit accuses Cigan of colluding with a claims administrator in a scheme that overcharged members. The lawsuit was filed last week in the United States District Court Eastern District of Pennsylvania by a Macy’s employee who was insured by Cigna. The complaint alleged that the insurer “misappropriates millions of dollars every year” from members by diverting administrative costs from vendors. The lawsuit also accused Cigna of falsifying Explanation of Benefits (EOB) forms to misrepresent charges from American Specialty Health, a company contracted by the insurer to process and administer healthcare claims and build provider networks, including chiropractors. Rather than paying for the administrative charges from ASH using plan fees and subscriber premiums, the complaint alleged Cigna disguises the charges as medical expenses. A Cigna spokesperson said they cannot comment on pending litigation.