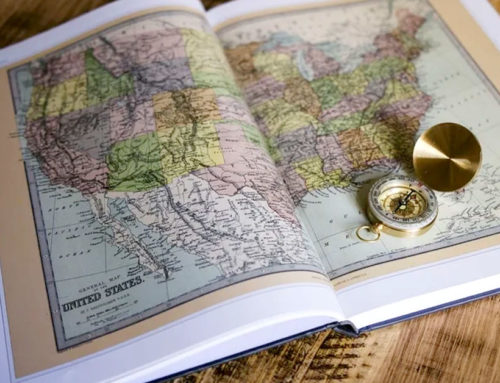
Forty four states filed against a group of 20 drug makers this week include Teva Pharmaceuticals, Inc., claiming price fixing, collusions and more. Meanwhile, another report uncovered that hospitals often charge double and sometimes even triple to private insurers over what Medicare would pay for the same procedures. The Trump Administration takes aim at ‘surprise billing’ and more in this week’s Innovation Partners BioBlog.

Many Hospitals Charge Double or Even Triple What Medicare Would Pay
Nationwide, private health insurance pays, on average, 2.4 times more than what Medicare would pay. Some states, such as Colorado, pay eight times more. A RAND study sheds light on the wide gap between what the federal government pays and what the private sector pays. The disparity shows how competition has faltered in a market where the costs of care are secret and hospital systems are increasingly consolidated.The lack of transparency, coupled with public outrage over rising hospital bills, has spurred calls for disclosure of the rates negotiated. This is the first time pricing information on a large group of individual hospitals has been made public.
READ MORE
Four Things to know about the IQVIA “Medicine Use and Spending” report
The new IQVIA report issued today highlights pricing, spending, and other cost drivers in the healthcare industry. Four findings are worth mentioning. After discounts and rebates, prices for brand medicines with patent exclusivity grew just 0.3 percent in 2018, slower than the rate of overall inflation. Spending on all medicines grew 4.5 percent in 2018 after discounts and rebates. $78 billion in net spending on brand medicines will be avoided due to loss of exclusivity and generic competition over the next five years. Lastly, medication prices are growing at slowest rate in years, but unfortunately, it doesn’t feel this way for many patients. The full report, at the link above, provides details and statistics from the complete study.
READ MORE
FDA’s finalized biosim interchangeability rules should give copycats a boost: analyst
The FDA has finalized a roadmap to allow biosimilars to be substituted at the pharmacy. Prior to the roadmap, biosims faced many hurdles. They can’t be automatically substituted at the pharmacy unless clinical data prove interchangeability with their reference products. The new roadmap aims to make it easier to substitution. Reviewers of the guidelines were pleasantly surprised and felt they were friendly towards biosim developers.
READ MORE
Forty four states accuse drug companies of price-fixing
Forty four states filed suit this week against a list of major pharmaceutical companies including Teva Pharmaceutical, Inc., alleging price fixing. The accusations include inflating prices, sometimes by more than 1,000 percent, and other means of colluding to fix prices. Teva is one of 20 companies accused of illegal policies.
READ MORE
Lilly plays up Cyramza’s biomarker edge in crowded liver cancer field
The FDA approved Lilly’s drug Cyramza for the treatment of liver cancer patients who have failed on Bayer’s Nexavar. Lilly has struggled to find its footing after Cyramza failed Stage 3 trials five years ago. Now, however, the FDA approval signals new life for the drug. Cyrama is clear to treat patients with high levels of the glycoprotein alpha-fetoprotein (AFP), a biomarker that can lead to worse outcomes. It affects about 40% of patients with hepatocellular carcinoma, the most common form of liver cancer.
READ MORE
Trump calls on Congress to take action on surprise billing
President Trump is taking aim at so-called “surprise billing” by pushing Congress to take action against the practice. Surprise billing often results from emergencies treated at hospitals out of a patient’s insurance network or when specialists not in a patient’s insurance network attend them at an in-network facility. For years, this practice has results in bills, sometimes over six figures, to people who thought their medical expenses were covered under their health insurance. Some of the suggestions are to provide up-front, clear billing to patients for elective services and balance billing to patients after emergency treatment.
READ MORE